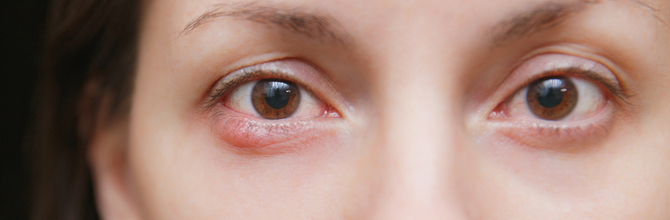
A stye – or hordeolum, as it’s known in the medical world – is a common type of eyelid infection, and most of us have one or two of them during our lifetime (i) (though some of us are more prone to getting them than others (ii)). But while styes can be painful, the good news is they’re not usually a sign of anything serious.
If you have a stye, you’ll usually have a small, red lump on the edge of your upper or lower eyelid that can develop into a little abscess that becomes swollen and filled with yellow pus. The infection and inflammation can sometimes spread, making your entire eyelid look red and swollen. This can make your eye feel more watery more than normal, but a stye shouldn’t usually affect your vision.
Other symptoms of a stye can include:
-
A crusty residue on the edge of the eyelid
-
Drooping eyelid
-
Eye itching
-
Sensitivity to light
-
Mucous discharge from the eye
-
Discomfort when you blink
-
A sensation of having something in your eye
Most people have one stye at a time, but it is possible for both eyes to be affected, or you may have more than one stye on the same eye (iii).
The bacterium that causes the infection is called Staphylococcus aureus, a common bacteria that can often be found on the surface of healthy skin where it usually doesn’t cause any problems (though if it gets into the skin it can cause infections such as spots and abscesses). If these bacteria get into the root (follicle) of an eyelash, however, they can infect it and cause a stye.
Glands in and around your eyelash follicles can also become infected and cause a stye. These are your sebaceous glands (also called Zeis glands), which produce oil to help lubricate your eyelashes, and apocrine glands (or Moll glands), which produce sweat that also helps prevent your eyelashes from drying out.
External vs internal styes
The most common type of stye is an external stye, which affects the outer edge of an eyelid. But you can get a stye on the inner surface of your eyelid too, called an internal stye.
Internal styes are much less common than external styes, and are the result of glands in the eyelid called meibomian glands becoming infected (meibomian glands secrete an oily fluid that helps keep your eyes and eyelids lubricated). Because the lump is on the inside of your eyelid you won’t be able to see it, though your eyelid may still look swollen. You may, however, be able to feel it, especially as the lump develops a yellow head, or you might simply experience a dull ache in your eyelid (internal styes are generally more painful than external ones).
The good news is most styes are harmless and tend to heal on their own in a week or so, and you shouldn’t usually need to see your GP when you have one.
Why do styes develop?
Often there’s no obvious reason why you get a stye, but if you rub your eyes a lot – especially without washing your hands – it can make getting a stye more likely. Poor eye hygiene increases the risk of getting a stye, so try to always do the following:
-
Remove eye make-up before going to bed and never share eye make-up with anyone else.
-
Disinfect your contact lenses before putting them in.
-
Wash your hands thoroughly before putting in contact lenses.
-
Dispose of eye make-up after its use-by date (if in doubt, replace every six months).
-
Never share towels or flannels with someone who has a stye, as the infection is contagious.
-
Blepharitis, an eye condition that causes inflammation of the eyelids.
-
Ocular rosacea (rosacea that affects your eyes, leading to symptoms such as irritation and sometimes also developing into blepharitis).
-
Seborrhoeic dermatitis (a common condition that can cause scaly, itchy and red skin).
Other sources suggest styes can also be more likely if you have diabetes, dry skin or are experiencing hormonal changes (iv).
Meanwhile, most styes don’t cause any problem, but occasionally the infection can spread and cause conjunctivitis, which is often called red eye or pink eye. Very rarely it can cause a very serious complication called orbital cellulitis that can destroy your vision and can potentially be life threatening. This is when the infection spreads to the whole eyelid as well as the tissues surrounding and behind the eye, causing sudden and often painful swelling of the eyelids, blurred vision, a high temperature and pain when you move your eye. If you develop any such symptoms, see a medical professional urgently.
Can styes be prevented?
While it’s not always possible to prevent a stye – since many develop for no reason – practising good eye hygiene is considered helpful. As well as following the steps outlined above, try to wash your hands thoroughly and often, especially if you tend to touch your face and eyes a lot (training yourself out of the habit of touching your face and eyes may also be useful).
If you have recurrent problems with blepharitis, treating it quickly may also help stop styes from developing.
How to treat a stye
Most styes don’t need any treatment, but you can easily look after one yourself at home. Here’s what you should do:
-
Relieve any swelling and soreness by applying a warm compress to the affected area of your eye. Take a clean flannel and soak it in warm water that has been boiled and left to cool a little. Wring out the flannel, then hold it against your eye for up to 10 minutes, and repeat three or four times a day.
This will help draw the pus in the stye to a head, which means it will burst and drain more quickly. However, don’t try to pop the head yourself, as this can make the infection spread or you may injure your eyelid while you’re doing it. -
Try to avoid wearing contact lenses or eye make-up until your stye has burst and healed. Also consider throwing away any mascaras, eyeliners or eye make-up applicators you were using just before or while the stye was developing, as they may be infected with bacteria.
-
Keep your eyelids as clean as possible. As well as using warm compresses, you can cleanse your eyelids by soaking a cotton wool pad in some warm water that has been boiled and left to cool, adding a drop or two of no-tears baby shampoo to the water first. Use the pad to gently cleanse your eyelid – if both eyes are affected, use separate pads. Make sure your hands have been washed thoroughly before you begin.
You can also use eyelid cleansing wipes – also sometimes called lid scrubs – which are available at pharmacies and online. -
If a stye is causing pain or discomfort, try taking a painkiller such as paracetamol or ibuprofen for relief.
Should you see your GP?
Unless a stye is causing problems, there shouldn’t be any reason to see your doctor. However, if you experience any of the following, see your GP as soon as possible:
-
Your eye becomes very painful or swollen
-
Your stye doesn’t heal within a few weeks
-
Your vision is affected
-
Your eyelid feels hot
-
You’ve noticed blisters forming on your eyelid
-
Your eye is so swollen you can’t open it
-
You get styes frequently
If necessary, your GP can burst an external stye with a sterilised needle or scalpel to drain the pus, or remove the affected eyelash, or they may refer you to a hospital eye specialist. You may be prescribed antibiotic eye drops or ointment if you also have conjunctivitis or if a stye persists, or antibiotic tablets if the infection is severe or the stye is very large.
Meanwhile, internal styes can be treated by draining and removing them under local anaesthetic (or, very occasionally, under general anaesthetic), and with antibiotic eye drops following the procedure.
Other eyelid and eyelash conditions
There are several other things that can cause eyelid and eyelash problems besides styes:
Chalazion
This is also a common eye condition that affects the eyelid, when a blockage of a meibomian gland causes a small fluid-filled cyst. The lump – or chalazion – that develops out of the cyst is firm and solid, and can persist for up to six months. It can cause mild pain or irritation at first – though chalazions aren’t usually as painful as styes – and there’s a small chance it can become infected. Vision isn’t usually affected, unless the chalazion becomes large and presses on the eye, causing blurry vision.
Up to half of people with a chalazion get better without any treatment (v), but as with a stye, a warm compress can provide relief if necessary. Persistent chalazions can be removed under local or general anaesthetic.
Other cysts
Besides chalazions there are other cysts that can develop around the eye, including cysts of Zeis (sebaceous gland cysts) and cysts of Moll (apocrine sweat gland cysts).
Milia
These are tiny white or pale yellow cysts that usually develop on the eyelid as well as around the eyes and nose, though they can affect any part of the body. Common in young babies, milia – which can also affect older children and adults – are filled with a protein called keratin and are harmless, clearing by themselves eventually (in babies they clear after just a few weeks but in adults they can last much longer). If troublesome, they can be removed by a dermatologist.
Xanthelasma
These are little yellowish flat bumps under the skin, usually on or around the upper or lower eyelids, and are thought to be caused by hyperlipidaemia (high levels of cholesterol or triglycerides). According to some researchers they can affect some people with normal cholesterol and triglyceride levels, but in such cases they’re often linked to a high body mass index or waist measurement (vi).
Trichiasis
Classed as a lid margin disorder, this is when your eyelashes grow in the wrong direction and point inwards towards the surface of your eye, causing irritation, redness and watering. Treatment includes having the affected eyelashes removed, but without treatment trichiasis can cause a corneal ulcer (an ulcer on the transparent front part of the eye).
Nutritional support for styes
Most styes are short lived, but there are natural ways of supporting your body as the infection resolves itself. Taking a good-quality multivitamin and mineral supplement may help make sure you’re getting all the nutrients your body needs – not just when you have an infection but at any time – especially if your diet isn’t always as healthy and balanced as it should be.
You may also want to consider one or more of the following:
High-strength fish oils
The omega-3 fatty acids found in oily fish such as salmon, sardines and mackerel are thought to have anti-inflammatory properties and there’s evidence they may be as effective as anti-inflammatory painkillers such as ibuprofen (vii). Another clinical trial suggests omega-3 supplements may be useful for those affected by blepharitis – which is a risk factor for styes – and meibomian gland dysfunction (viii). One source also claims eye specialists often recommend a diet high in omega-3 fatty acids to reduce the risk of eye problems (ix).
Astaxanthin
This plant-based antioxidant – classed as a carotenoid – has also been found to reduce inflammation (x). Astaxanthin is a particularly powerful antioxidant (xi) and is derived from a freshwater microalgae called Haematococcus pluvialis (it’s the red pigment in the algae that give certain fish and shellfish their red or pink colour – salmon and lobster, for instance).
You can get astaxanthin in your diet by eating foods such as salmon, lobster, shrimp, crawfish and crab, but it’s unlikely you’d be able to eat enough of these foods to get the amount of astaxanthin needed to see any real vision benefits. Taking a high-quality supplement, however, would provide a more beneficial dose of astaxanthin – plus it’s a good option for anyone who doesn’t like eating fish or seafood.
You can read more about astaxanthin and how it benefits other aspects of vision health in our article Astaxanthin and Eye Health: The Potential Benefits.
Evening primrose oil
Thanks to the fact that it contains gamma-linolenic acid (GLA) – an omega-6 fatty acid – evening primrose oil may also be helpful, as GLA has also been found to have an anti-inflammatory action (xii). GLA is made in the body from linoleic acid, another omega-6 fat, but can also be found in trace amounts in green leafy vegetables and nuts, as well as in evening primrose oil.
Turmeric
You may know it as the spice that gives curry its flavour and distinctive yellow colour, but turmeric is also an increasingly popular nutritional supplement thanks to its active ingredient curcumin. Indeed, evidence suggests curcumin may benefit a range of inflammatory conditions (xiii). Studies also suggest curcumin may be as effective as conventional anti-inflammatory drugs such as ibuprofen for pain relief (xiv).
There’s lots more information on eye conditions in our vision health hub. Or to find out more about a range of other health conditions, visit our dedicated health library.
References:
-
Available online: https://www.moorfields.nhs.uk/condition/styes
-
Available online: http://www.irishhealth.com/article.html?con=195
-
Available online: https://patient.info/eye-care/swollen-eyelid/stye
-
Available online: https://my.clevelandclinic.org/health/diseases/17658-sty-stye/diagnosis-and-tests
-
Available online: https://patient.info/eye-care/swollen-eyelid/chalazion
-
Chan. C.C., Lin. S.J., Hwang. J.J., et al. Xanthelasma is not associated with increased risk of carotid atherosclerosis in normolipidaemia. Int J Clin Pract. (2008 Feb). 62(2):221-7. Available online: https://www.ncbi.nlm.nih.gov/pubmed/18036167?dopt=Abstract
-
Maroon. J.C., Bost. J.W. Omega-3 fatty acids (fish oil) as an anti-inflammatory: an alternative to nonsteroidal anti-inflammatory drugs for discogenic pain. Surg Neurol. (2006 Apr). 65(4):326-31. Available online: https://www.ncbi.nlm.nih.gov/pubmed/16531187
-
Macsai. M.S. The Role of Omega-3 Dietary Supplementation in Blepharitis and Meibomian Gland Dysfunction. Trans Am Ophthalmol Soc. (2008). 106:336-356. Available online: https://pubmed.ncbi.nlm.nih.gov/19277245-the-role-of-omega-3-dietary-supplementation-in-blepharitis-and-meibomian-gland-dysfunction-an-aos-thesis/
-
Available online: https://www.allaboutvision.com/nutrition/fatty_acid_1.htm
-
Miyachi M. et al., Anti-inflammatory effects of astaxanthin in the human gingival keratinocyte line NDUSD-1. J Clin Biochem Nutr. 2015 May;56(3):171-178. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4454080/
Park JS. et al., Astaxanthin decreased oxidative stress and inflammation and enhanced immune response in humans. Nutr Metab (Lond). 2010;7:18. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2845588/ -
Miki W. et al., Biological functions and activities of animal carotenoids. Pure Appl. Chem. 1991;63:141-6. Available online: https://www.researchgate.net/publication/244741723_Biological_Functions_and_Activities_of_Animal_Carotenoids
-
Kapoor. R., Huang. Y.S. Gamma linolenic acid: an antiinflammatory omega-6 fatty acid. Curr Pharm Biotechnol. (2006 Dec). 7(6):531-4. Available online: https://www.ncbi.nlm.nih.gov/pubmed/17168669
-
Aggarwal. B.B., Harikumar. K.B. Potential therapeutic effects of curcumin, the anti-inflammatory agent, against neurodegenerative, cardiovascular, pulmonary, metabolic, autoimmune and neoplastic diseases. Int J Biochem Cell Biol. (2009 Jan). 41(1):40-59. Available online: https://www.ncbi.nlm.nih.gov/pubmed/18662800
-
Gupta. S.C., et al. Therapeutic Roles of Curcumin: Lessons Learned from Clinical Trials. AAPS J. (2013 Jan). 15(1): 195–21. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3535097
-
Kuptniratsaikul. V., et al. Efficacy and safety of Curcuma domestica extracts compared with ibuprofen in patients with knee osteoarthritis: a multicenter study. Clin Interv Aging. (2014). 9: 451–458. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3964021
Related Posts
Disclaimer: The information presented by Nature's Best is for informational purposes only. It is based on scientific studies (human, animal, or in vitro), clinical experience, or traditional usage as cited in each article. The results reported may not necessarily occur in all individuals. Self-treatment is not recommended for life-threatening conditions that require medical treatment under a doctor's care. For many of the conditions discussed, treatment with prescription or over the counter medication is also available. Consult your doctor, practitioner, and/or pharmacist for any health problem and before using any supplements or before making any changes in prescribed medications.

Christine
Christine Morgan has been a freelance health and wellbeing journalist for almost 20 years, having written for numerous publications including the Daily Mirror, S Magazine, Top Sante, Healthy, Woman & Home, Zest, Allergy, Healthy Times and Pregnancy & Birth; she has also edited several titles such as Women’ Health, Shine’s Real Health & Beauty and All About Health.
View More



