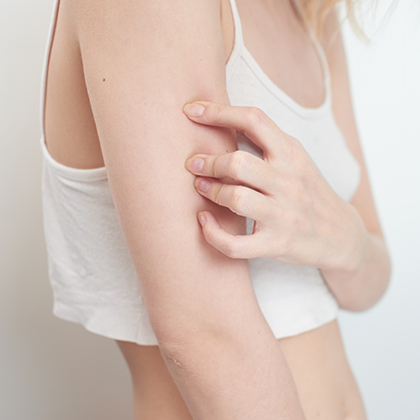
There are a number of other names for urticaria, including hives, welts, nettle rash and weals. All refer to a raised rash that can be very itchy and blotchy. It can be just a few millimetres in size and confined to one part of the body, or it can spread and cover much larger areas. The rash, which can be pink or red, comprises swellings (weals) that are round or oval in shape and sometimes surrounded by a red flare. They commonly affect the face or arms, hands, fingers, legs, feet and toes. Most frequently these weals disappear fairly quickly – sometimes within a few hours and often within eight to 12 hours, with weals lasting for more than 24 hours being rare.
The weals, however, are often replaced by new ones, and the rash can last for days or even months. Other skin conditions, such as eczema or psoriasis, can sometimes present similar symptoms to urticaria, so it’s important to recognise the differences between them.
What causes it?
Urticaria is caused by tiny blood vessels called capillaries in the affected area opening up and leaking fluid into the skin, with the accumulating fluids making the skin red, swollen and itchy. This change in the blood vessels is thought to be a reaction to high levels of substances called chemical messengers – the most well-known of which is histamine – being released in the skin.
The most common form of urticaria is often caused by allergies. Some of the things thought to trigger the release of histamine include:
-
Certain foods (such as eggs, milk, fish and nuts)
-
Dust
-
Pollen
-
Certain medicines (painkillers known as non-steroidal anti-inflammatory drugs – or NSAIDs – can cause symptoms in some people, as can medicines used to treat high blood pressure called ACE inhibitors)
Urticaria complications
Around one in five people will be affected by ordinary urticaria at some point, says the NHS, with children often affected as well as women aged 30 to 60 and those with a history of allergies (i). Many urticaria sufferers will also develop a condition called angioedema. This is often described as a deeper form of urticaria, as the swelling affects the deeper layers of your skin.
If you have angioedema, the rash can affect your eyelids, lips, hands, feet, genitals and sometimes the inside of the mouth (sometimes the tongue and throat can also be affected). The rash can last longer with angioedema too, and it can take up to three days for the swelling to die down. A more rare form of angioedema is called hereditary angioedema, which as its name suggests tends to run in families (between one in 10,000 and one in 50,000 people are affected worldwide (ii)). This condition is caused by a blood protein deficiency, and a severe attack can be life threatening if it isn’t treated.
Urticaria can also be an early symptom of anaphylaxis, which is a severe and potentially life-threatening allergic reaction. Other symptoms of anaphylaxis include swollen lips, eyes, hands and feet, wheezing and breathing difficulties, lightheadedness, stomach pain, nausea and vomiting. If you think you or someone else is experiencing anaphylaxis, call 999 immediately.
Urticaria: acute vs chronic
Urticaria can be either acute – in which your rash usually clears completely within six weeks or less – or chronic, where the rash lasts or comes and goes for longer.
According to the National Institute for Health and Care Excellence (NICE), 20 per cent of people will have acute urticaria at some point in their lives, while two to three per cent of people will have chronic urticaria (iii). Both acute and chronic urticaria cause the same type of rash, and you may develop angioedema if you’re affected by either type of the condition (around 50 per cent of people with chronic urticaria also have regular episodes of angioedema (iv)). Both acute and chronic urticaria are the result of histamine and other chemicals being released into the skin.
Acute urticaria
In addition to allergies to some types of food, certain medicines and insect bites and stings, acute urticaria is thought to be triggered by a reaction to a viral infection in some people. This means you may develop a rash if you have a cold or flu, or another type of viral infection such as glandular fever or hepatitis B. However the cause of the rash is only identified in about half of cases of acute urticaria (v). And unfortunately, some people have recurring bouts of acute hives.
Indeed, the cause of the rash isn’t known in more than half of cases of acute urticaria. But thankfully, it’s also likely that if you have an episode of acute urticaria, it won’t come back a second time.
Chronic urticaria
The triggers for chronic urticaria are less clear, however. Experts aren’t really sure what causes it, but it’s thought around a third to half of all cases are related to a problem with the immune system (or what is called an autoimmune reaction) (vi). This may be because chronic urticaria can sometimes happen in combination with other autoimmune conditions such as rheumatoid arthritis, thyroid disease or lupus.
Unlike acute urticaria, however, chronic urticaria can come and go for months or even years. Some things may make it worse, such as alcohol, caffeine and stress.
Physical urticarias
For some people, the thing that triggers their urticaria is some form of physical stimulation. Like ordinary urticaria a physical urticaria can be acute or chronic, but triggered by factors such as heat, exercise, cold, light, pressure on the skin and even water:
Dermatographism
This is when you get a rash on your skin when it has been firmly stroked – around five per cent of people will develop this at some point in their lives (vii). Dermatographism literally means skin writing. If you ‘write’ on the skin by applying pressure with your finger or another object, whatever you write will appear as a rash. Any part of the skin can be affected, though the palms of your hands, soles of your feet and your scalp are less likely to have a rash. People find their dermatographism is more prominent when they are hot – after a hot bath or shower, for instance. And while it can be very itchy (though not always), the rash usually lasts less than an hour.
Dermatographism (also called dermographism and dermotographia) usually starts when you’re a young adult, but in most cases it improves over the years (vii).
Cholinergic urticaria
Also called heat bumps, this type of urticarial rash develops when you sweat – for instance, when you’re exercising, when you’re hot, when you’re under a lot of emotional stress or when you eat spicy food. You normally experience small itchy bumps within just a few minutes of starting to sweat, and the rash can last from half an hour to an hour or more. The rash usually affects the upper part of the body including the chest, back and arms, and can sometimes be accompanied by breathlessness and wheezing.
Solar urticaria
A rare form of urticaria causing redness, itching and weals, this is triggered when an affected person’s skin is exposed to sunlight.
Cold urticaria
This type of urticaria isn’t common, with a rash developing after you’ve been exposed to cold, including rain, cold wind and cold water. The rash affects parts of the skin that have become cold, so if caused by swimming in cold water for example, it can cover large areas of the body (for this reason, people with cold urticaria are advised not to swim in cold water). Experts aren’t sure whether the rash is caused by the cold itself, or the skin warming up after being exposed to cold (vii).
Aquagenic urticaria
If your skin develops small weals whenever it comes into contact with water of any temperature, your condition is called aquagenic urticaria. However, this condition is very rare.
Delayed pressure urticaria
Not a common condition, this can affect people with ordinary urticaria. It can develop four to six hours after part of your skin has been subjected to persistent pressure – after wearing tight clothes, for example, or after a long journey wearing a seat belt.
Treating urticaria
Mild cases of acute urticaria don’t usually need any medical treatment, as the symptoms often improve within a few days. During that time, taking cool baths or showers may soothe your skin. You could also try applying calamine lotion – which is available over the counter – to soothe the affected area. However, using calamine lotion can cause more itching if you leave it on for too long. Another topical treatment you could try is menthol in aqueous cream, which may also help with itching and keep the skin cool.
If your symptoms are causing discomfort you could try taking antihistamine tablets – available at pharmacies without a prescription – to reduce the itching. More severe cases of acute urticaria are often treated with a short course of steroid tablets.
Chronic urticaria treatments
If you know what triggers your chronic urticaria, avoiding it wherever possible is the obvious way to keep your condition under control. Some people with chronic urticaria also find the following useful:
-
Staying cool (especially at night)
-
Avoiding hot baths, alcohol, caffeine and – where possible – stress
-
Wearing loose rather than tight clothes
If you have chronic urticaria you may be advised to take antihistamines – particularly the older type of antihistamines that can make you drowsy, as they could help you to get a better night’s sleep (some people take a non-sedating antihistamine during the day and a sedating one at night). Antihistamines are also often used to help reduce the symptoms of angioedema, but they aren’t usually effective in cases of delayed pressure urticaria.
Calamine lotion and menthol in aqueous cream can help with chronic urticaria too. Other treatments sometimes used in cases of chronic urticaria include leukotriene receptor antagonists (medication that can help reduce swelling of the skin), and ciclosporin (an immune suppressant medication).
A newer treatment called omaluzimab – which is given as an injection – is also thought to be effective in cases that haven’t responded to antihistamines. Omaluzimab may reduce antibodies that are believed to be involved in urticaria.
Diet may also play a part in some cases of chronic urticaria, with substances found in foods called vasoactive amines and salicylates thought to trigger the condition. However these are found in a wide range of foods, so the best approach may be to keep a food diary to work out which particular foods may be causing the problem.
Natural remedies for urticaria
In addition to keeping your skin cool and looking into whether some of the foods you eat may be causing your urticaria, there are some natural remedies you can try:
Quercetin
Belonging to a group of plant substances called flavonoids, quercetin is thought by some to be a powerful antioxidant that may help reduce inflammation. It’s often used by natural health practitioners as a treatment for allergies – including urticaria – as lab tests have shown it may block the release of histamine from certain immune cells (viii). Quercetin is available as nutritional supplements as well as in red wine, grapefruit, onions, apples, black tea, leafy green vegetables and beans.
Fish oils
The omega-3 essential fatty acids found in oily fish have been shown to help reduce inflammation (ix). Found in fish such as salmon, sardines, pilchards, mackerel, trout and fresh tuna, fish oils are also available as nutritional supplements for those who cannot or do not want to eat fish.
Vegetarians and vegans can now benefit from omega-3 supplements too, thanks to the availability of products that contain the natural triglyceride (TG) form of omega-3 (this is sourced from plant organisms called microalgae rather than fish).
Anthocyanidins
These antioxidant compounds are found in dark-skinned fruits such as blueberries, cranberries, raspberries, blackberries and red grapes, as well as vegetables such as red cabbage, red onions and aubergines. Anthocyanidins also belong to a group of plant chemicals called flavonoids. As well as having antioxidant and anti-inflammatory properties, flavonoids have been shown to have a natural antihistamine action (x). This suggests they may help control allergic reactions, including urticaria.
Iron
There is some evidence that some cases of chronic urticaria may be improved by taking iron supplements. Indeed, in one study, people with chronic urticaria who also had low iron levels took an iron supplement for one to two months. At the end of the study period some of the volunteers experienced significant improvements in their condition, with many reporting their urticaria had disappeared completely (xi). Your GP can prescribe an iron supplement if you’re diagnosed with iron-deficiency anaemia. Iron supplements are also widely available without prescription. However, some forms of iron can cause stomach upsets, including constipation. To prevent this, choose a form of iron that’s easy on the stomach in a supplement, such as iron citrate. Iron is also often included in decent levels in good-quality multivitamin and mineral supplements.
Urticaria can be very uncomfortable, but trying some of the remedies above can help to alleviate the itchiness. To find more information on common health conditions and advice on treatments, visit the dedicated resources in our health library.
References:
-
Available online: https://www.nhsinform.scot/illnesses-and-conditions/skin-hair-and-nails/urticaria-hives
-
Available online: https://www.nhsinform.scot/illnesses-and-conditions/skin-hair-and-nails/angioedema
-
Available online: https://cks.nice.org.uk/urticaria#!backgroundSub:2
-
Available online: https://patient.info/allergies-blood-immune/allergies/angio-oedema
-
Available online: https://patient.info/doctor/urticaria-pro
-
Available online: https://www.nhsinform.scot/illnesses-and-conditions/skin-hair-and-nails/urticaria-hives#causes-of-urticaria-hives
-
Available online: https://patient.info/skin-conditions/hives-inducible-urticaria
-
Ogasawara. H, Middleton. E Jr. Effect of selected flavonoids on histamine release (HR) and hydrogen peroxide (H2O2) generation by human leukocytes [abstract]. J Allergy Clin Immunol. 1985 ;75(suppl):184.
Middleton. E Jr. Effect of flavonoids on basophil histamine release and other secretory systems. Prog Clin Biol Res. 1986 ;213:493-506.
Micek J et al., Quercetin and Its Anti-Allergic Immune Response. Molecules. 2016 May 12;21(5). Pii: E623.Available online: https://www.ncbi.nlm.nih.gov/pubmed/27187333
Simopoulos. AP. Omega-3 fatty acids in inflammation and autoimmune disease. J AM Coll Nutr. 2002 Dec;21(6):495-505.
Calder PC., Omega-3 fatty acids and inflammatry processes: from molecules to man. Biochem Soc Trans. 2017 Oct 15;45(5):1105-1115.Available online: https://www.ncbi.nlm.nih.gov/pubmed/28900017
Park. HH, Lee. S et al. Flavonoids inhibit histamine release and expression of proinflammatory cytokines in mast cells. Arch Pharm Res. 2008 Oct;31(10):1303-11.
Guarneri. F, Guarneri. C, Cannavo. SP. Oral iron therapy and chronic idopathic urticaria: sideropenic urticaria? Dermatol Ther. 2014 Jul-Aug;27(4):223-6.
Related Posts
Disclaimer: The information presented by Nature's Best is for informational purposes only. It is based on scientific studies (human, animal, or in vitro), clinical experience, or traditional usage as cited in each article. The results reported may not necessarily occur in all individuals. Self-treatment is not recommended for life-threatening conditions that require medical treatment under a doctor's care. For many of the conditions discussed, treatment with prescription or over the counter medication is also available. Consult your doctor, practitioner, and/or pharmacist for any health problem and before using any supplements or before making any changes in prescribed medications.

Christine
Christine Morgan has been a freelance health and wellbeing journalist for almost 20 years, having written for numerous publications including the Daily Mirror, S Magazine, Top Sante, Healthy, Woman & Home, Zest, Allergy, Healthy Times and Pregnancy & Birth; she has also edited several titles such as Women’ Health, Shine’s Real Health & Beauty and All About Health.
View More