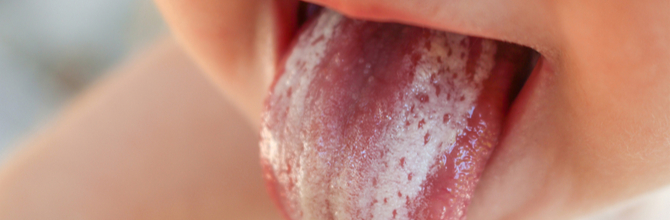
If there’s an unusual white rash or white patches inside your mouth – typically on your tongue or the inside of your cheeks – there’s a chance you may have an infection called oral thrush.

Oral thrush is also called oral candidiasis or oral candiasis because it’s caused by a group of fungal yeasts called Candida (the species that most commonly causes oral thrush is Candida albicans, though other Candida species such as C. glabrata, C. krusei and C. tropicalis can sometimes be the culprits).
White spots in the mouth are the classic oral thrush symptom, but you may also experience one or more of the following:
-
Yellow or grey larger spots in the mouth called plaques (these may form when several white spots join together)
-
Red and usually painless spots left when a white spot is wiped or knocked off
-
Redness in the mouth and throat
-
A burning sensation in the mouth
-
Sore, cracked and red areas on the outside of your mouth, usually in the corners of the mouth where the upper and lower lips meet
-
Distorted sense of taste or unpleasant taste in the mouth
-
Redness where dentures sit
Pain isn’t always a feature of mild oral thrush infections, but they may make your mouth feel sore, which can cause discomfort while eating and drinking. And sometimes the infection can also spread to your tonsils, the back of your throat or your oesophagus (gullet).
Why do some people get oral thrush?
The Candida fungi live in most people’s mouths in small amounts and are a part of normal oral microflora (they can also live in other parts of the body including the digestive tract, the ears, the eyes, the nose and the vagina). In low numbers these fungi are usually harmless. But in certain conditions they can multiply, causing an overgrowth that can trigger oral thrush symptoms. This can happen in the following situations:
-
If you’re taking antibiotics – the antibiotics kill both harmful and harmless bacteria in your mouth but not Candida, which can multiply more easily when bacteria levels are low.
-
If you wear dentures (particularly if you leave your dentures in overnight or your wear poorly fitting dentures that rub your gums). The National Institute for Health and Care Excellence (NICE) states around 50 - 70 per cent of denture wearers are predisposed to oral thrush infection (i).
-
If you use steroid inhalers (for asthma, for example) or take steroid tablets.
-
If you have a persistently dry mouth (see our guide to dry mouth for more information).
-
If you have Sjogren’s syndrome, which can cause dry mouth.
-
If you have diabetes.
-
If you have problems with your immune system (such as when taking immunosuppressive medicines, for instance, or if you have HIV/AIDS or are having chemotherapy treatment for cancer).
-
If you have severe anaemia or are deficient in iron, folate or vitamin B12.
-
If you smoke (according to NICE, smokers are nearly seven times more likely to have oral thrush than non-smokers (i)).
-
If you have generally poor health or are frail (up to 10 per cent of debilitated older people are thought to be affected (i)).
-
If you use antibacterial mouthwash excessively.
In healthy adults, however, oral thrush isn’t common. Meanwhile, if you have symptoms including white patches on the tongue or inside of your cheeks it could be a sign of another problem, such as:
Lichen planus
This is a rash that can affect various parts of the body including the inside of the mouth (in the mouth it causes white patches on the gums, tongue or inside of the cheeks, plus you may experience a burning or stinging sensation in your mouth). Other symptoms of lichen planus include clusters of red blotches on the arms, legs or body and bald patches on the scalp.
Leukoplakia
A white patch on your tongue that doesn’t go away could be a sign that you have leukoplakia. The patches can also appear on the inside of the cheeks, on the gums or on the floor or roof of your mouth.
Mouth ulcers
Painful blister-like sores inside the mouth, including on the tongue, can be mouth ulcers.
Geographic tongue
This common condition causes blotchy red patches on the tongue that have a whiteish border. The patches can become painful, especially when you eat anything acidic.
How is oral thrush treated?
There are several treatments for oral thrush, including antifungal gels, liquids, tablets and capsules.
Topical antifungal treatments are usually the first thing your doctor may recommend – you simply apply a small amount of gel or place a few drops of liquid in your mouth on the affected area several times a day for one or two weeks. You can buy these remedies over the counter from pharmacies.
Tablets and capsules are usually prescribed in more severe cases of oral thrush, or for people who are more likely to develop more serious symptoms because they have a weakened immune system, for example. You may also have to take antifungal tablets or capsules if you’ve tried using a gel or liquid but there hasn’t been any improvement in your symptoms.
Meanwhile, if another medication you’ve been taking has caused the problem – antibiotics, for example – your doctor may consider adjusting the dosage or prescribing an alternative medicine to help the oral thrush symptoms clear up.
How to help yourself
When being treated for oral thrush there are a few things you could do in the meantime to help relieve the symptoms and clear up the infection. These include the following:
-
Rinse your mouth with soothing salt water (dissolve half a teaspoon of salt in a cup of warm water). A similar solution made with baking soda instead of salt may also be useful.
-
Use a very soft toothbrush that’s gentle on your mouth, then throw it away and use a new toothbrush when the infection has cleared up.
-
Eat live yoghurt, as it contains live bacteria (research suggests live bacteria may help reduce the growth of Candida albicans (ii)).
-
Avoid overusing mouthwashes or spray, as these may interfere with the normal balance of bacteria in your mouth.
Oral thrush in babies
Oral thrush is common in babies. According to NICE, about five per cent of newborns are affected by oral thrush, increasing to 14 per cent in month-old babies and then decreasing gradually thereafter (i). Some babies also have recurring bouts of oral thrush.
Experts believe Candida multiplies in babies’ mouths because their immune systems aren’t fully developed, meaning they cannot control the levels of the fungi (iii). Babies who are taking antibiotics may also be more susceptible to developing oral thrush, or they may be affected if they’re being breastfed and their mothers are taking antibiotics.
The symptoms of oral thrush in babies are similar to those in adults, namely white spots developing on a baby’s tongue and in their mouth, causing a sore mouth. This can – but doesn’t always – make a baby refuse to feed properly or they may drool a lot more than usual. Other symptoms include redness inside the mouth and cracks in the corners of the mouth.
If they’re having a mild case of oral thrush, a baby doesn’t always need any treatment, and the infection may clear up on its own within just a few days. If the symptoms persist, however, an antifungal gel or drops may be prescribed by your doctor.
What can you do?
There isn’t always a reason why a baby develops oral thrush, and it’s not usually caused by poor hygiene. There are, however, several things you can do that may help prevent it:
-
Sterilise any feeding equipment such as bottles and teats regularly, as well as dummies or any toys your baby puts in their mouth (teething rings, for example).
-
Try giving your baby some water to drink straight after a feed, as Candida may thrive on any milk that stays in their mouth after feeding.
-
Inform your doctor or midwife if you have any pain or discharge during breastfeeding, as these could be a sign of a nipple yeast infection that could be transmitted to your baby during feeding.
Can oral thrush be prevented?
There’s not always anything you can do to stop getting a bout of oral thrush, but you may be able to reduce your risk of developing it by doing the following:
-
Rinse your mouth with water after eating.
-
Practise good oral health – brush your teeth twice a day with a fluoride toothpaste and clean between your teeth regularly using dental floss, dental tape or interdental brushes.
-
If you have no or not very many teeth of your own, brush your gums, tongue and the inside of your mouth with a soft toothbrush twice daily.
-
Always see your dentist for a check-up as often as they recommend.
-
If you wear dentures, take them out every night and clean them thoroughly, as wearing dentures all of the time is one of the most common causes of oral thrush (your dentist can tell you the best way to keep your dentures clean). Also if your dentures don’t fit properly, see your dentist for advice.
-
Consider quitting if you’re a smoker. Try over-the-counter products such as nicotine patches, gum and lozenges if you need help with managing your cravings.
-
Take frequent sips of water throughout the day if you’re taking any medication that causes dry mouth or if you have a medical condition that causes dry mouth (Sjogren’s syndrome, for example).
-
If you use a steroid inhaler to treat the symptoms of asthma, rinse your mouth with water after each dose (using a spacer – a plastic tube that attaches to an inhaler – can also help). Ask your doctor or pharmacist to check your inhaler technique, and make sure you’re on the lowest dose of steroid medication needed to control your asthma. Also try cleaning your inhalers after each use.
-
Try to make sure you manage your condition effectively if you’re living with diabetes, as good blood sugar control may help prevent oral thrush as well as other infections. Treating anaemia or low vitamin B12, folate or iron levels as your doctor advises may also help prevent any further bouts.
-
Consider limiting the amount of sugar in your diet, as there is some evidence that eating fewer sugary foods may help prevent Candida overgrowth (though studies have so far only looked at the role of dietary sugar in vaginal thrush) (iv).
Natural support for oral thrush
If oral thrush is making your mouth sore, you may avoid eating certain foods or you may have a reduced appetite in general. This could mean you’re not getting the range of nutrients from your diet that your body needs. You can, however, make sure your nutrient intake is adequate by taking a good-quality multivitamin and mineral supplement. Look for a supplement that includes good levels of iron, folic acid and vitamin B12, as low levels of all three nutrients are associated with the development of oral thrush.
Other natural supplements you may find useful include the following:
Live bacteria
Many natural health practitioners recommend supplements containing live bacteria for oral thrush, as bacteria such as acidophilus have been found to help treat the symptoms because they stop Candida growing (ii). As well as supplements you could try eating more foods that are naturally rich in live bacteria, such as live yoghurt and kefir, a fermented milk drink.
Garlic
A compound in garlic called allicin is believed to have antifungal properties, which may explain why garlic is often recommended as a natural treatment for oral thrush.
Vitamin C
Oral thrush may be associated with a deficiency or low levels of iron, folate and vitamin B12, but researchers believe vitamin C deficiency may be to blame too. In one study involving elderly hospitalised people, vitamin C deficiency was found to be one of the most significant risk factors for oral thrush, alongside taking antibiotics, poor oral hygiene and wearing dentures (v). You can boost your intake of vitamin C by eating plenty of fruits and vegetables, particularly berries, blackcurrants, broccoli, tomatoes, peppers and kiwifruit, or by taking a good-quality vitamin C supplement.
If you have oral thrush it can affect your quality of life, but this guide should help to make it a little easier.
References:
-
Available online: https://cks.nice.org.uk/topics/candida-oral/background-information/prevalence/
-
Matsubara. V.H., et al. Probiotic lactobacilli inhibit early stages of Candida albicans biofilm development by reducing their growth, cell adhesion, and filamentation. Appl Microbiol Biotechnol. (2016 Jul). 100(14):6415-26. Available online: https://www.ncbi.nlm.nih.gov/pubmed/27087525
-
Available online: https://patient.info/childrens-health/oral-thrush-in-babies
-
Horowitz. B.J., Edelstein. S.W., Lippman. L. Sugar chromatography studies in recurrent Candida vulvovaginitis. J Reprod Med. (1984 Jul). 29(7):441-3. Available online: https://www.ncbi.nlm.nih.gov/pubmed/6481700 [Accessed 21 Feb. 2019].
-
Paillaud. E., et al. Oral candidiasis and nutritional deficiencies in elderly hospitalised patients. Br J Nutr. (2004 Nov). 92(5):861-7. Available online: https://www.ncbi.nlm.nih.gov/pubmed/15533276 [Accessed 21 Feb. 2019].
Related Posts
Disclaimer: The information presented by Nature's Best is for informational purposes only. It is based on scientific studies (human, animal, or in vitro), clinical experience, or traditional usage as cited in each article. The results reported may not necessarily occur in all individuals. Self-treatment is not recommended for life-threatening conditions that require medical treatment under a doctor's care. For many of the conditions discussed, treatment with prescription or over the counter medication is also available. Consult your doctor, practitioner, and/or pharmacist for any health problem and before using any supplements or before making any changes in prescribed medications.

Christine
Christine Morgan has been a freelance health and wellbeing journalist for almost 20 years, having written for numerous publications including the Daily Mirror, S Magazine, Top Sante, Healthy, Woman & Home, Zest, Allergy, Healthy Times and Pregnancy & Birth; she has also edited several titles such as Women’ Health, Shine’s Real Health & Beauty and All About Health.
View More

